Tribal Health in India
by Dr. Sunil Kumar
Tribal population is an important segment of India’s population living in different parts of the country. One-third of the world’s tribal and indigenous population, which is, more than 104 million tribal population live in India (Census 2011). Perhaps, they are the only native inhabitants of in the country.
There are 705 different tribes, which constitute 8.6 per cent of the total country’s population. Odisha has the largest number of notified Scheduled Tribe (62), followed by Karnataka (50) Maharashtra (42) and Madhya Pradesh has the 4th place with 43 notified tribes.
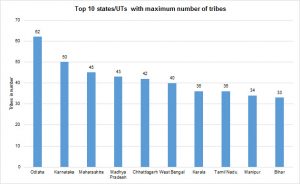
Figure1
Source: Report of the High-Level Committee on Socio-Economic, Health and Educational Status of Tribal Communities of India 2014
As far as concentration of ST population is concerned, Madhya Pradesh has 14.7 per cent (over 153 lakh) of total ST population, which is the largest concentration of ST population in terms of numbers in any Indian state, followed by Maharashtra (over 10 million), Odisha and Rajasthan (over 9 million each).
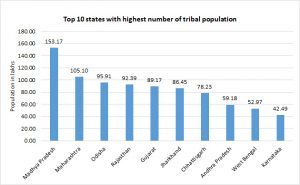
Figure 2
Source: Report of the High-Level Committee on Socio-Economic, Health and Educational Status of Tribal Communities of India 2014
The concentration of tribal population mainly located in different regions in the country. Predominantly, it was highly concentrated in North-Eastern region apart from the numbers, Mizoram has 94.43 per cent tribal population in the state, followed by Nagaland (86.47%), Meghalaya (86.14%) and Arunachal Pradesh with 68.78 per cent tribal population.
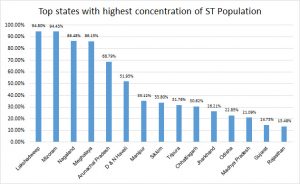
Figure 3
Source: Report of the High-Level Committee on Socio-Economic, Health and Educational Status of Tribal Communities of India 2014
However, Lakshadweep was leading in tally with 94.80 per cent tribal population but its actual representation is less than 65 thousand in numbers, whereas Mizoram’s tribal population was more than 10 lakhs.
Tribal Health
Tribal people in India commonly called as Adivasi, the term Adivasi made up from two words Adi (from the beginning) and Vasi (inhabitant), derives from the Hindi, which means a set of people or group living from the beginning. There are few other terms as Vanavasi (“forest dwellers) or Girijan (“hill people”), by which tribal people identified.
The above terms to tribal population given on the bases of their primitive existence and geographic location of inhabitation. Forest and hilly region are the favourite place for the tribal population; they largely associate with forest ecosystem and try to fulfil their need and requirement within the same. Out of total tribal population (104.30 lakhs), only 10.03 per cent living in urban area, an overselling majority of the tribal population (89.97%) still living in the rural and remote periphery, as per Census, 2011.
In many ways, the tribal population in India struggling with many development indicators. Altogether, 40.6 per cent ST population lived below the poverty line as against 20.5 per of the non-tribal population in the county, by and large poverty is main obstacle to get quality health services, accessibility to health services are second. Tribal population largely filed to manage at both the fronts.
Health Indicator among tribal population
Largely, statistics on the health conditions of different tribal communities are not available, whatever the data available evidencing the health status of Scheduled Tribes is available at the aggregate level.
IIPS conducted a study, in which they estimated the life expectancy of the tribal and non-tribal population in India, shows ST population in India has 63.9 years, as against 67 years life expectancy for the general population. The Rapid Survey on Children 2013-14 reveals that more than 30 per cent ST women get married before they turn 18. It is much noticeable that near about 50 per cent adolescent ST girl (between 15 to 19 years) are underweight and high prevalence anaemia cause to death for 17 to 46 per cent of maternal cases deaths. According to NSSO 2014, 27 per cent of tribal women still delivers at home, which is the highest among all population group.
Figure 4 shows, 40 per cent illness happen to tribal population due to some or other type of infection, followed by respiratory diseases (18 %), Non-communicable and Musculoskeletal diseases (10 % each). Mental illness and neurological disorder (5%) also increased significantly in the tribal population.
Malaria usually transmitted the bite of an infected Anopheles mosquito and it is a life-threatening disease. The 20 per cent of country’s population living in tribal, hill, hard-to-reach or inaccessible areas, constitute almost 80 per cent of malaria case. India accounts for 8 per cent of the tribal population and contributes to 30 per cent of malaria cases.
Animals Attacks
As, it is already discussed in the inception of tribal health that they are inherently habitant of the forest ecosystem, where chances to conflict with the animals are always higher. India has highest snakebite mortality in the world, which is between 45 to 50 thousand annually or about 125 people per day.
Health infrastructure
In India, there are 0.7 physicians per thousand people and a majority of the Indian need to travel about 20 km to access the services of the hospital. As per the Ministry of Health, there are around 6 to 6.5 lakh medical practitioners available in India, which need to be double by 2020 to maintain the required ratio of one doctor per thousand population.
Figure 5, shows that there is a shortfall of 6646 sub-centres in tribal areas across the country. More than 12 hundred PHCs need to establish and at least 300 other CHCs will be helpful to cater the need tribal population in India.
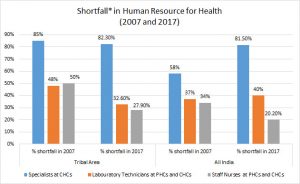
As far as a shortfall of human resources is concerned, figure 6 shows that there were 85 per cent specialists lacking at CHCs in tribal areas until the year 2007, which is not decreased much (82.30%) in 2017. The need for specialists at CHCs almost similar across India during the year 2017. There was a need of 50 per cent Staff Nurses at PHCs and CHCs in 2007 in tribal areas, which subsequently reduced to 27.90 per cent. In the corresponding category, they need 20.20 per cent of staff nurses in all India in 2017.
As per the Report: Tribal Health India-2018, following ten burdens of tribal health in India
- Communicable diseases, Maternal and child health problems and malnutrition continue to prevail
- Non-communicable diseases including mental stress and addiction are rapidly increasing
- Injuries due to accidents, snake and animal bites and violence in conflict situations
- Difficult natural conditions arising due to geographic terrain, distances and harsh environments
- Worse social-economic determinants, especially in education, income, housing, connectively, water and sanitation
- Poor quality and inappropriate health care service with low access and coverage, low output and outcomes
- Severe constraints in health human resources at all levels; the professionals from outside are unwilling to serve in tribal areas, and the local potential human resources are not trained and utilized by the health system.
- The legitimate and needed financial share for tribal health not allocated or used in most of the states. There is a lack of transparent accounting of the actual expenditure of tribal health.
- Lack of data, monitoring and evaluation that masks the above-mentioned problems.
- Political disempowerment of tribal people from the individual to the national level that exacerbates these problems. There is little inclusion of tribal people in the planning, priority setting and in execution.